Peripheral Vascular Disease
Blanket Health We Have Your Medical Needs Covered!
- Home
- Peripheral Vascular Disease
Unveiling Peripheral Vascular Disease: Causes, Symptoms, and Management
The circulatory system is a complex network of blood vessels that ensures the transportation of oxygen and nutrients throughout the body. While we often focus on the central components of this system, such as the heart and major arteries, it’s equally important to understand the peripheral vascular system. Peripheral vascular disease (PVD) is a group of disorders that affect these peripheral blood vessels, potentially causing a range of health issues. In this comprehensive article, we will explore the world of peripheral vascular disease, including its causes, symptoms, diagnosis, and treatment options.
The Peripheral Vascular System: An Overview
The peripheral vascular system encompasses all blood vessels outside the heart and brain. It includes arteries, veins, and capillaries that extend to every part of the body, serving essential functions such as oxygen delivery, waste removal, and temperature regulation.
Key components of the peripheral vascular system include:
- Arteries: These vessels carry oxygen-rich blood away from the heart to supply the body’s tissues and organs. Arteries have thick, elastic walls to withstand the force of the heartbeat.
- Veins: Veins return deoxygenated blood from the body’s tissues back to the heart. They have thinner walls and often have one-way valves to prevent blood from flowing backward.
- Capillaries: These tiny, thin-walled vessels connect arteries and veins and allow for the exchange of oxygen, nutrients, and waste products between blood and tissues.
- Lymphatic System: While not part of the vascular system, the lymphatic system plays a vital role in maintaining fluid balance and immune function. Lymphatic vessels transport lymph, a clear fluid that carries white blood cells and waste products.
Understanding Peripheral Vascular Disease (PVD)
Peripheral vascular disease is a collective term for various conditions that affect the peripheral blood vessels, primarily the arteries. These disorders can lead to reduced blood flow, which may result in tissue damage and a range of symptoms. Two common types of PVD are peripheral artery disease (PAD) and peripheral venous disease (PVD), each with distinct characteristics.
- Peripheral Artery Disease (PAD): PAD primarily affects the arteries, causing a buildup of fatty deposits (atherosclerosis) that narrows and hardens the arterial walls. This narrowing restricts blood flow to the extremities, most commonly the legs. Reduced blood supply can result in symptoms like leg pain, cramping, and ulcers.
- Peripheral Venous Disease (PVD): PVD, also known as chronic venous insufficiency, primarily affects the veins in the legs. It occurs when the one-way valves in the veins become damaged or fail, leading to blood pooling in the lower extremities. Symptoms of PVD may include leg swelling, pain, and skin changes like ulcers and discoloration.
Causes and Risk Factors of Peripheral Vascular Disease
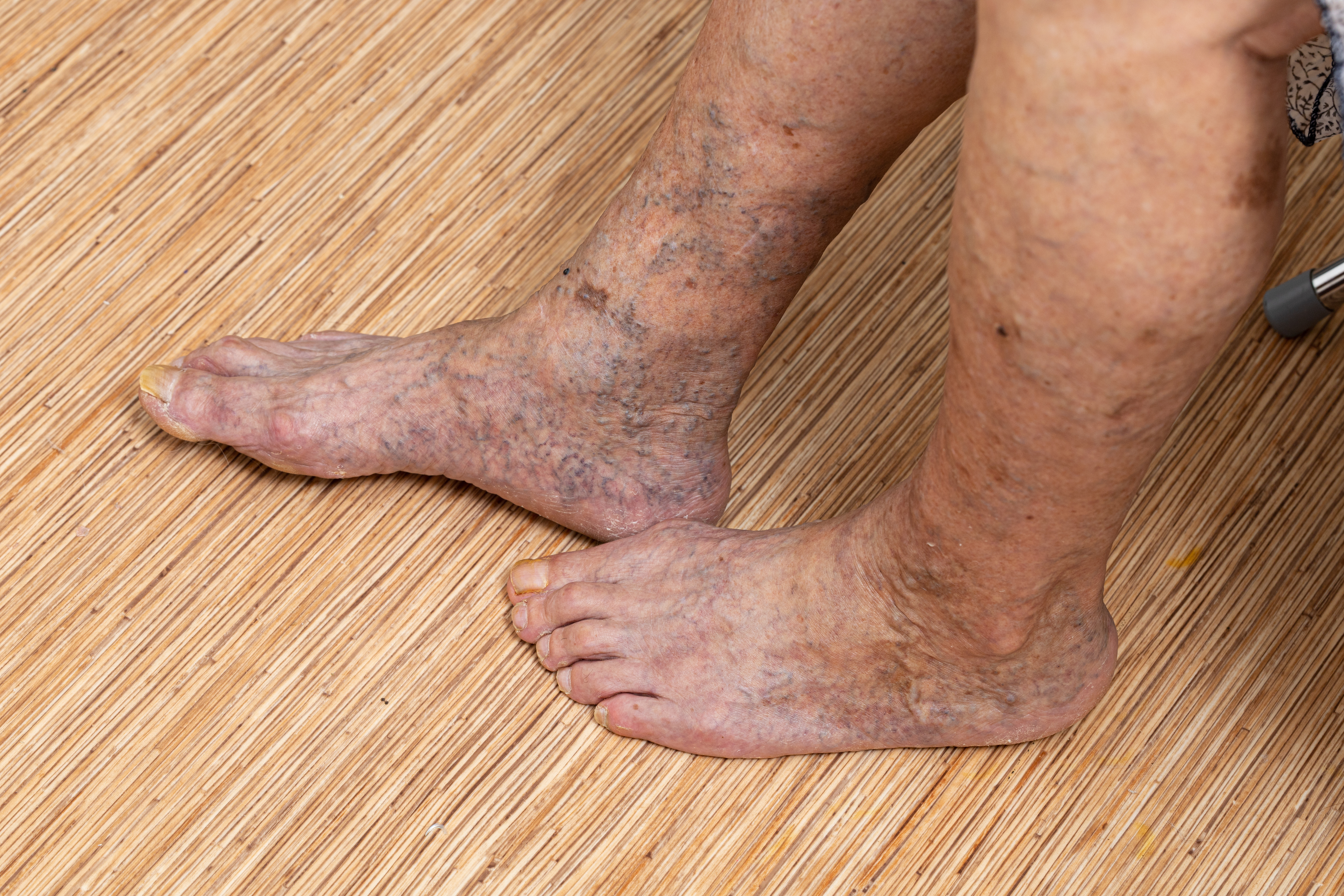 Several factors contribute to the development of PVD. These include:
Several factors contribute to the development of PVD. These include:
- Atherosclerosis: The most common cause of PAD, atherosclerosis involves the buildup of fatty plaques in the arteries, narrowing the blood vessels.
- Age: PVD risk increases with age, particularly in individuals over 50.
- Smoking: Smoking is a significant risk factor for PVD, as it damages blood vessels and accelerates atherosclerosis.
- Diabetes: High blood sugar levels can harm blood vessels, increasing the risk of PAD and PVD.
- High Blood Pressure: Uncontrolled hypertension can damage blood vessels over time.
- High Cholesterol: Elevated cholesterol levels contribute to the formation of atherosclerotic plaques.
- Obesity: Excess weight places additional strain on the circulatory system, increasing PVD risk.
- Sedentary Lifestyle: Lack of physical activity can lead to reduced blood flow and muscle deconditioning.
- Family History: A family history of PVD may indicate a genetic predisposition.
- Other Medical Conditions: Conditions such as kidney disease, autoimmune disorders, and blood clotting disorders can also increase PVD risk.
Symptoms of Peripheral Vascular Disease
The symptoms of PVD can vary depending on the type and severity of the condition. Common symptoms include:
- Claudication: Pain, cramping, or discomfort in the legs during physical activity, which typically improves with rest. This is a hallmark symptom of PAD.
- Numbness or Weakness: Reduced blood flow can lead to numbness or weakness in the affected extremities.
- Cold Feet or Hands: Poor circulation can result in cold extremities.
- Skin Changes: In advanced cases, skin changes may occur, such as shiny or discolored skin, thickened toenails, or ulcers that are slow to heal.
- Leg Swelling: PVD may cause fluid retention and swelling in the legs and ankles, particularly in cases of chronic venous insufficiency.
- Rest Pain: Severe PAD can cause pain even at rest, often in the feet or toes.
Diagnosis and Evaluation
Diagnosing PVD involves a combination of medical history, physical examination, and diagnostic tests. Common evaluation methods include:
- Ankle-Brachial Index (ABI): This non-invasive test compares blood pressure measurements in the arms and ankles to assess blood flow in the legs.
- Duplex Ultrasound: This imaging technique uses sound waves to visualize blood flow and identify any blockages or abnormalities.
- CT Angiography or Magnetic Resonance Angiography: These imaging studies provide detailed images of blood vessels and can help identify areas of narrowing or blockage.
- Arteriography: Invasive arteriography involves injecting contrast dye into blood vessels and taking X-ray images to identify blockages or other abnormalities.
Treatment and Management of Peripheral Vascular Disease
Treatment for PVD aims to improve blood flow, manage symptoms, and reduce the risk of complications. Depending on the severity and type of PVD, treatment options may include:
- Lifestyle Modifications: Lifestyle changes such as quitting smoking, maintaining a healthy weight, and adopting regular exercise can improve blood flow and overall vascular health.
- Medications: Medications may be prescribed to manage risk factors like high blood pressure, cholesterol levels, and diabetes. Antiplatelet drugs, such as aspirin, can help prevent blood clots.
- Peripheral Angioplasty and Stenting: These minimally invasive procedures involve opening narrowed or blocked arteries with the use of a balloon or stent to restore blood flow.
- Bypass Surgery: In severe cases of PAD, bypass surgery may be necessary to reroute blood flow around blocked arteries.
- Compression Therapy: For PVD with venous insufficiency, compression stockings can help reduce swelling and improve blood flow in the legs.
- Wound Care: In cases of chronic venous insufficiency, proper wound care is essential to prevent infection and promote healing of ulcers.
Peripheral vascular disease is a complex group of conditions that can impact the peripheral blood vessels, leading to a range of symptoms and health risks. Early diagnosis and appropriate management are crucial to improving blood flow, reducing symptoms, and preventing complications. If you suspect you may have PVD or are experiencing related symptoms, it is essential to consult with a healthcare provider for a comprehensive evaluation and personalized treatment plan. By addressing risk factors and managing PVD effectively, individuals can maintain vascular health and enjoy a higher quality of life.
Living With Peripheral Vascular Disease
Living with Peripheral Vascular Disease (PVD) can present numerous challenges that impact daily life and overall well-being. However, it is important to recognize that with the right approach and a few lifestyle changes, individuals with PVD can significantly enhance their quality of life. In this article, we will explore strategies and practical steps to improve one’s life while managing this condition.
Peripheral Vascular Disease encompasses a group of conditions that affect the blood vessels outside the heart and brain. A common underlying factor is atherosclerosis, the buildup of fatty deposits in the arteries. This can lead to reduced blood flow to the limbs, particularly the legs, resulting in symptoms like leg pain, numbness, and difficulty walking. While living with PVD may seem daunting, it is essential to understand that effective management strategies can help individuals lead fulfilling and meaningful lives. Regular physical activity plays a pivotal role in managing PVD. Although it might appear counterintuitive to exercise when experiencing leg pain, consistent physical activity can significantly improve blood circulation, alleviate symptoms, and enhance overall cardiovascular health. Low-impact activities such as walking, swimming, or stationary cycling are excellent choices for individuals with PVD. It is crucial to start slowly and gradually increase the duration and intensity of workouts under the guidance of a healthcare provider. Engaging in regular exercise not only benefits physical health but also contributes to improved mood and mental well-being.

Maintaining a healthy diet is another fundamental aspect of managing PVD and enhancing quality of life. A well-balanced diet can support overall health and minimize the risk factors associated with PVD. It is advisable to focus on incorporating foods rich in nutrients such as fruits, vegetables, whole grains, lean proteins, and healthy fats into your daily meals. Reducing the intake of saturated and trans fats, sodium, and added sugars can also contribute to better cardiovascular health. Consulting with a registered dietitian or nutritionist can provide personalized guidance on dietary choices and meal planning tailored to your specific needs. Smoking is a significant risk factor for PVD, as it not only damages blood vessels but also accelerates the progression of atherosclerosis. If you are a smoker, quitting is one of the most effective steps you can take to improve your quality of life while living with PVD. It can be challenging, but various smoking cessation programs, support groups, and resources are available to assist individuals in their journey toward a smoke-free life. Quitting smoking not only benefits cardiovascular health but also reduces the risk of numerous other health issues.
Effective management of PVD involves regular medical check-ups and open communication with healthcare providers. Regular visits allow for the monitoring of the condition’s progression, adjustments to treatment plans, and early intervention when necessary. Additionally, it provides an opportunity to address any concerns or questions you may have about managing PVD effectively. Building a trusting and collaborative relationship with your healthcare team is essential in navigating the challenges of living with PVD. Incorporating stress management techniques into your daily routine can also significantly enhance your quality of life. Stress can exacerbate symptoms of PVD and negatively impact overall health. Techniques such as deep breathing exercises, meditation, mindfulness, or yoga can help reduce stress levels and promote relaxation. Engaging in hobbies, spending time with loved ones, and seeking emotional support when needed are equally important aspects of managing stress.
Compression therapy, which involves wearing specially designed stockings or socks, can be beneficial for individuals with PVD, particularly in cases of chronic venous insufficiency. These garments help reduce swelling, improve blood flow in the legs, and alleviate discomfort. Consulting with a healthcare provider can help determine if compression therapy is suitable for your specific condition and needs. When living with PVD, it is essential to practice meticulous wound care, especially if you have ulcers or skin changes in the affected areas. Proper wound care helps prevent infection, promotes healing, and reduces the risk of complications. Cleaning wounds, applying prescribed medications, and keeping them covered with sterile dressings are crucial steps in managing skin issues associated with PVD.
Maintaining a positive outlook and a strong support system are invaluable resources for individuals living with PVD. Connecting with others who share similar experiences through support groups or online communities can provide emotional support, practical advice, and a sense of camaraderie. It is essential to remember that you are not alone in your journey. In conclusion, living with Peripheral Vascular Disease presents unique challenges, but it is possible to lead a fulfilling and meaningful life with the condition. By adopting a proactive approach that includes regular physical activity, a healthy diet, smoking cessation, stress management, and close collaboration with healthcare providers, individuals can significantly enhance their quality of life. Additionally, seeking support from loved ones and connecting with peers facing similar challenges can provide a strong foundation for managing PVD effectively and maintaining overall well-being.
Peripheral Vascular Disease FAQ
1. What is Peripheral Vascular Disease (PVD)?
- Peripheral Vascular Disease, often referred to as PVD, is a group of conditions that affect the blood vessels outside the heart and brain. It primarily involves atherosclerosis, a buildup of fatty deposits in the arteries, leading to reduced blood flow to the limbs, especially the legs. This reduced blood flow can result in symptoms like leg pain, numbness, and difficulty walking.
2. What are the risk factors for developing PVD?
- Several factors increase the risk of developing PVD, including:
- Smoking: Smoking is a significant risk factor for PVD as it damages blood vessels.
- Diabetes: Individuals with diabetes are at a higher risk due to the potential damage to blood vessels caused by high blood sugar levels.
- High blood pressure: Uncontrolled hypertension can harm blood vessels over time.
- High cholesterol: Elevated cholesterol levels contribute to the formation of atherosclerotic plaques.
- Age: The risk of PVD increases with age, particularly in those over 50.
3. What are the common symptoms of PVD?
- Symptoms of PVD can vary but often include:
- Claudication: Pain, cramping, or discomfort in the legs during physical activity, which typically improves with rest.
- Numbness or weakness: Reduced blood flow can lead to numbness or weakness in the affected extremities.
- Cold feet or hands: Poor circulation can result in cold extremities.
- Skin changes: In advanced cases, skin changes may occur, such as shiny or discolored skin, thickened toenails, or ulcers that are slow to heal.
- Leg swelling: PVD may cause fluid retention and swelling in the legs and ankles, particularly in cases of chronic venous insufficiency.
4. How is Peripheral Vascular Disease diagnosed?
- Diagnosis typically involves a combination of medical history, physical examination, and diagnostic tests. Common evaluation methods include:
- Ankle-Brachial Index (ABI): A non-invasive test that compares blood pressure measurements in the arms and ankles to assess blood flow in the legs.
- Duplex Ultrasound: This imaging technique uses sound waves to visualize blood flow and identify blockages or abnormalities.
- CT Angiography or Magnetic Resonance Angiography: Imaging studies that provide detailed images of blood vessels and can help identify areas of narrowing or blockage.
- Arteriography: An invasive procedure that involves injecting contrast dye into blood vessels and taking X-ray images to identify blockages or other abnormalities.
5. What are the treatment options for Peripheral Vascular Disease?
- Treatment for PVD aims to improve blood flow, manage symptoms, and reduce the risk of complications. Depending on the severity and type of PVD, treatment options may include:
- Lifestyle modifications: These include quitting smoking, maintaining a healthy weight, and adopting regular exercise to improve blood circulation.
- Medications: Medications may be prescribed to manage risk factors like high blood pressure, cholesterol levels, and diabetes.
- Procedures: Minimally invasive procedures, such as angioplasty and stenting, may be performed to open narrowed or blocked arteries.
- Bypass surgery: In severe cases of PAD, bypass surgery may be necessary to reroute blood flow around blocked arteries.
- Compression therapy: For PVD with venous insufficiency, compression stockings can help reduce swelling and improve blood flow in the legs.
It is essential to consult with a healthcare provider for a proper diagnosis and personalized treatment plan if you suspect you have PVD or are experiencing related symptoms.
