Breast Cancer Screening
Blanket Health We Have Your Medical Needs Covered!
- Home
- Breast Cancer Screening
The Power of Prevention: Understanding Breast Cancer Screening
Breast cancer is a formidable adversary, affecting millions of women worldwide. However, advances in medical science have significantly improved our ability to detect this disease at an early stage, greatly enhancing the chances of successful treatment. Breast cancer screening plays a pivotal role in this endeavor, offering women a proactive approach to managing their health. In this article, we will explore breast cancer screening comprehensively, delving into its significance, methods, guidelines, and the importance of informed decision-making.
The Significance of Breast Cancer Screening
Breast cancer screening is a set of medical tests and examinations designed to detect breast cancer before symptoms manifest. Its importance lies in the fact that early detection significantly improves the prognosis and survival rates of individuals diagnosed with breast cancer. By identifying cancer at an earlier, more treatable stage, screening can lead to less aggressive treatments, better outcomes, and a higher quality of life for patients.
Methods of Breast Cancer Screening
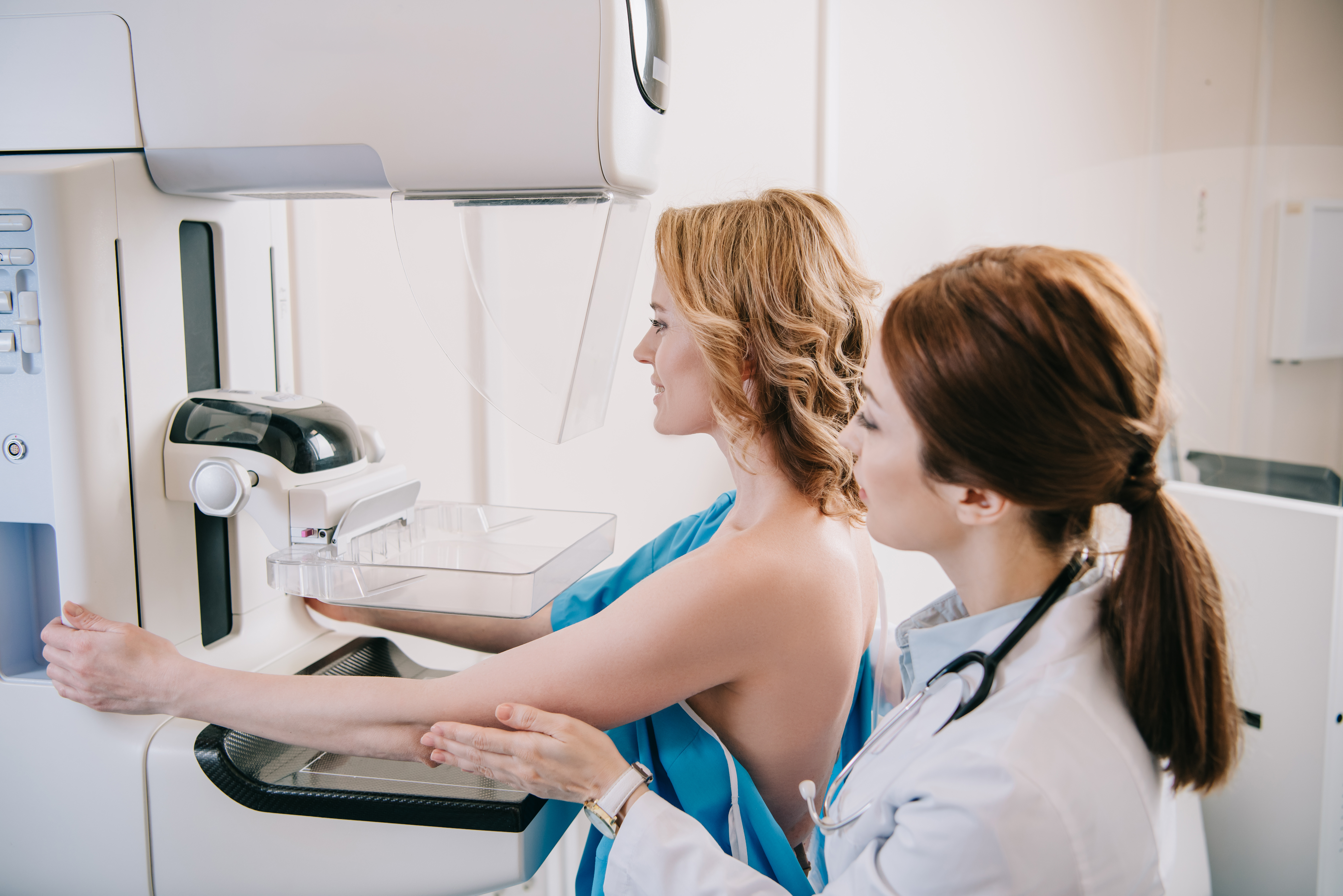 There are two primary methods of breast cancer screening:
There are two primary methods of breast cancer screening:
1. Mammography: Mammography is the most widely used screening tool for breast cancer. It involves taking X-ray images of the breast tissue. Digital mammography, 3D mammography (tomosynthesis), and contrast-enhanced mammography are some of the advanced techniques that enhance detection accuracy. Regular mammograms can detect tumors too small to be felt during a breast exam.
2. Clinical Breast Examination (CBE): Clinical breast examination is a physical examination of the breasts conducted by a healthcare provider. During a CBE, the healthcare provider assesses the breasts for lumps, changes in size or shape, or other abnormalities. While it’s an important part of breast cancer screening, it’s often used in conjunction with mammography for a more comprehensive assessment.
Breast Self-Examination (BSE)
Breast self-examination is another important aspect of breast cancer awareness. While it’s not a formal screening method, it encourages women to become familiar with their own breast tissue. Regular self-examinations can help individuals detect any changes or abnormalities in their breasts, which can then be promptly discussed with a healthcare provider.
Guidelines for Breast Cancer Screening
Breast cancer screening guidelines may vary depending on factors like age, family history, and personal risk factors. Some general guidelines include:
- Mammography: The American Cancer Society recommends that women with an average risk of breast cancer start annual mammograms at age 45 and continue until age 54. Afterward, they can choose to have mammograms every two years.
- Clinical Breast Examination (CBE): The American Cancer Society suggests that clinical breast examinations be performed as part of a periodic health exam, preferably every three years for women in their 20s and 30s, and annually for women 40 and older.
It’s essential to note that recommendations may differ between organizations, so it’s advisable to discuss your individual screening plan with your healthcare provider. In some cases, such as when there is a family history of breast cancer or other risk factors, more frequent or specialized screening may be recommended.
Informed Decision-Making
Breast cancer screening is a personal choice, and individuals should make informed decisions based on their unique circumstances. It’s crucial to consider factors such as family history, age, and overall health when determining the appropriate screening regimen. Additionally, one should weigh the potential benefits of early detection against the possibility of false positives, overdiagnosis, and the emotional toll of unnecessary biopsies or treatments.
Furthermore, individuals should engage in open and informed discussions with their healthcare providers to determine the best screening plan for their situation. This dialogue should consider the potential benefits, limitations, and risks of screening. Informed decision-making empowers individuals to take control of their health and make choices aligned with their values and preferences.
Breast cancer screening is a powerful tool in the fight against breast cancer. By detecting the disease at an early stage, it can significantly improve treatment outcomes and ultimately save lives. However, it’s essential to approach screening with a balanced perspective, taking into account individual risk factors, screening guidelines, and informed decision-making. Engaging in regular breast self-examinations, discussing screening options with healthcare providers, and following recommended guidelines can help individuals stay proactive in their breast health and contribute to a brighter future in the battle against breast cancer.
Preparing For Your Breast Cancer Screening
Preparing for a breast cancer screening involves several key steps to ensure that the process goes smoothly and that you obtain accurate and meaningful results. Here’s a guide on how to prepare for a breast cancer screening:
Schedule an Appointment: The first step is to schedule your breast cancer screening appointment. Depending on your age, risk factors, and the specific screening method recommended for you, this could involve booking a mammogram, clinical breast examination (CBE), or both. Contact your healthcare provider or a breast health clinic to arrange the appointment.
Choose the Right Time: When scheduling your mammogram or CBE, consider scheduling it during a time when your breasts are less likely to be tender or swollen. This typically means avoiding the week before your menstrual period, as breast discomfort may be more pronounced during this time.
Wear the Right Attire: On the day of your screening, wear comfortable clothing that can be easily removed from the waist up. It’s often more convenient to wear a two-piece outfit or a top with a skirt or pants instead of a one-piece dress.
Skip Deodorant and Powders: Avoid using deodorant, talcum powder, or creams on your underarms or breasts on the day of your mammogram. These substances can sometimes interfere with the quality of the mammogram images.
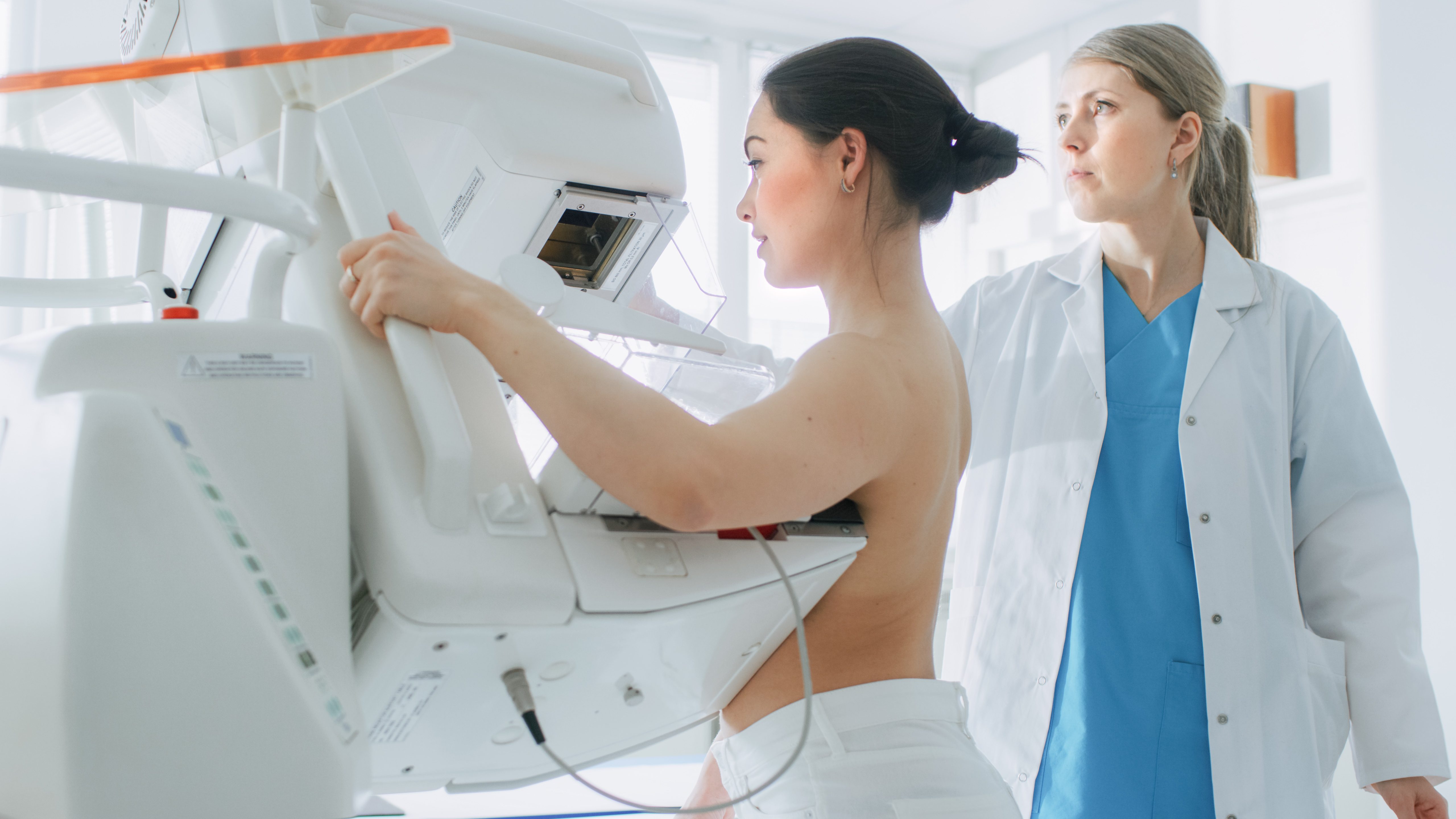 Bring Previous Imaging: If you have had previous mammograms or breast imaging at a different facility, try to obtain these records and bring them to your appointment. These records can serve as a baseline for comparison and provide valuable information to the radiologist.
Bring Previous Imaging: If you have had previous mammograms or breast imaging at a different facility, try to obtain these records and bring them to your appointment. These records can serve as a baseline for comparison and provide valuable information to the radiologist.
Inform Your Healthcare Provider: During your appointment, be sure to inform your healthcare provider about any breast-related concerns, symptoms, or changes you may have noticed. This information can help guide the screening and evaluation process.
Relax and Stay Calm: Many individuals may feel anxious before a breast cancer screening, especially if it’s their first time. It’s entirely normal to experience nervousness, but try to stay as relaxed as possible. The healthcare professionals conducting the screening are experienced and trained to ensure your comfort.
Ask Questions: If you have any questions or concerns about the screening process, don’t hesitate to ask your healthcare provider or the medical staff. Understanding what to expect can alleviate anxiety and enhance your overall experience.
Plan for Follow-Up: Be prepared for the possibility of follow-up tests or additional imaging if abnormalities or areas of concern are identified during the initial screening. Remember that not all findings indicate cancer, and further evaluation may be needed to provide a definitive diagnosis.
Stay Informed: After your screening, discuss the results with your healthcare provider. If your results are normal, continue to follow recommended screening guidelines. If further evaluation or treatment is required, work closely with your healthcare team to develop a comprehensive plan.
Breast cancer screening is a proactive step in maintaining your breast health. By adequately preparing for your screening and actively participating in the process, you contribute to early detection and, ultimately, better outcomes in the fight against breast cancer.
Important Breast Cancer Screening Guidelines To Know
Breast cancer screening guidelines provide recommendations on when and how often individuals should undergo screening tests for the early detection of breast cancer. These guidelines are typically established by medical organizations and are based on extensive research and evidence. It’s essential to note that screening guidelines may vary slightly between organizations, and individual factors like age, family history, and personal risk should also be considered when determining the appropriate screening plan. Here is an overview of some widely recognized breast cancer screening guidelines:
- Mammography Guidelines:
- American Cancer Society (ACS): The ACS recommends that women with an average risk of breast cancer should begin annual mammograms at age 45. Starting at age 55, they can choose to continue with annual mammograms or switch to mammograms every two years. Women between ages 40 and 44 are encouraged to make an informed decision about when to start screening based on their individual risk factors.
- U.S. Preventive Services Task Force (USPSTF): The USPSTF recommends biennial mammography screening for women aged 50 to 74. They suggest that women in their 40s should make individual decisions based on their risk factors and preferences.
- Clinical Breast Examination (CBE) Guidelines:
- The American Cancer Society no longer recommends routine clinical breast examinations for breast cancer screening for average-risk women. Instead, they emphasize that women should be familiar with how their breasts look and feel and promptly report any changes or concerns to their healthcare providers.
- Breast Self-Examination (BSE):
- The American Cancer Society no longer recommends routine breast self-examinations for breast cancer screening. However, they suggest that women should be aware of how their breasts normally look and feel and promptly report any changes to their healthcare providers.
- Individualized Screening:
- For individuals with a higher risk of breast cancer due to factors like a strong family history or known genetic mutations (e.g., BRCA1 or BRCA2), more frequent and specialized screening may be recommended. This could include earlier initiation of mammography and additional imaging modalities like breast MRI.
It’s crucial to understand that breast cancer screening guidelines are subject to updates as new research and evidence emerge. Additionally, individual factors play a significant role in determining the most appropriate screening plan. Therefore, it’s advisable to discuss your specific circumstances with your healthcare provider. They can help you make an informed decision about when to start screening, how often to screen, and which screening methods are most suitable for you based on your age, family history, and other relevant factors. Regular discussions with your healthcare provider and adherence to recommended screening guidelines can contribute to the early detection of breast cancer, increasing the chances of successful treatment and better outcomes.
Ways to Screen for Breast Cancer At Home Before You Make Your Appointment
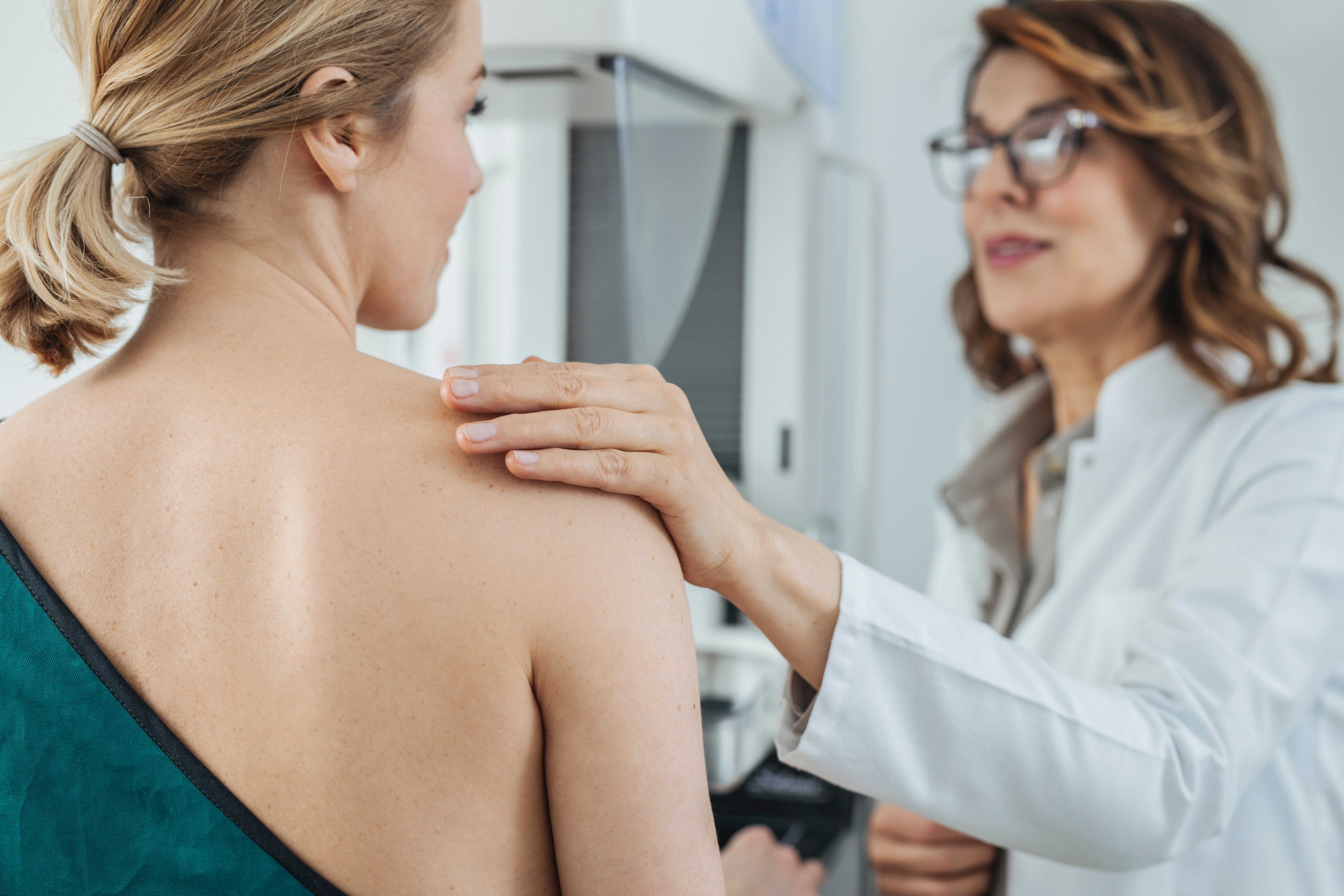 Performing a breast self-examination (BSE) at home is a vital aspect of breast health awareness. It allows individuals, especially women, to monitor their breasts for any changes or abnormalities between clinical breast examinations and mammograms. To conduct a BSE effectively, begin by choosing the right time—preferably about a week after your menstrual period starts when your breasts are less likely to be swollen or tender. Stand in front of a mirror with your arms at your sides and visually inspect your breasts for any visible changes in size, shape, or symmetry. Note any skin alterations, dimpling, or puckering, and look for changes in the position or appearance of your nipples.
Performing a breast self-examination (BSE) at home is a vital aspect of breast health awareness. It allows individuals, especially women, to monitor their breasts for any changes or abnormalities between clinical breast examinations and mammograms. To conduct a BSE effectively, begin by choosing the right time—preferably about a week after your menstrual period starts when your breasts are less likely to be swollen or tender. Stand in front of a mirror with your arms at your sides and visually inspect your breasts for any visible changes in size, shape, or symmetry. Note any skin alterations, dimpling, or puckering, and look for changes in the position or appearance of your nipples.
Next, raise your arms above your head and repeat the visual examination. Continue to observe for any differences between your breasts and any skin or nipple abnormalities. For the manual examination, lie down on your back and place a small pillow or folded towel under your right shoulder. Raise your right arm behind your head to help spread out the breast tissue. Using the pads of your three middle fingers on your left hand, gently feel for lumps or abnormalities in your right breast. Start at the outer edge and move inward, employing a circular motion. Cover the entire breast, moving up and down until you have assessed the entire area.
Repeat this process for your left breast. When performing the manual examination, remember to use varying degrees of pressure—light for the tissue closest to the skin, medium for the middle layers, and firm for the tissue nearest to the chest wall. Finally, check your nipples for any discharge by gently squeezing each nipple to see if any fluid, other than breast milk, is present. Should you notice any unusual discharge or any changes in the nipples during your BSE, it’s crucial to promptly contact your healthcare provider for further evaluation. To ensure effectiveness, make breast self-examination a monthly habit, ideally on the same day each month, and report any changes or concerns to your healthcare provider.
Breast Cancer Screening FAQ
1. When should I start getting regular breast cancer screenings?
Answer: The recommended age to start regular breast cancer screenings can vary depending on guidelines and individual risk factors. In general, the American Cancer Society recommends that women with an average risk of breast cancer should start annual mammograms at age 45. However, some organizations suggest considering mammograms starting at age 40. It’s essential to discuss your specific situation, including family history and risk factors, with your healthcare provider, who can help determine the appropriate age to begin screening.
2. How often should I have mammograms?
Answer: The frequency of mammograms can vary depending on your age, risk factors, and specific guidelines. Typically, women with an average risk of breast cancer are advised to have annual mammograms starting at age 45 or 50. However, some organizations may recommend biennial (every two years) mammograms for women aged 50 to 74. Women in their 40s may have mammograms annually or every two years, depending on individual circumstances. The recommended frequency may change as you age, so consult with your healthcare provider to establish the most suitable screening schedule for you.
3. Are there any alternative breast cancer screening methods besides mammography?
Answer: While mammography is the primary screening tool for breast cancer, other methods, such as breast MRI and ultrasound, may be recommended for specific situations. Breast MRI is often used for individuals at high risk of breast cancer due to factors like a strong family history or known genetic mutations (e.g., BRCA1 or BRCA2). Ultrasound may be used as a supplementary tool for further evaluation of specific findings identified during mammography. Your healthcare provider will determine if additional screening methods are necessary based on your individual risk factors.
4. Can men get breast cancer, and should they undergo screening?
Answer: Yes, men can develop breast cancer, although it’s less common than in women. Men with a family history of breast cancer or specific risk factors may be advised to undergo breast cancer screening, which can include mammography and clinical breast examinations. However, the frequency and necessity of screening for men are determined on a case-by-case basis, and individuals should consult with their healthcare providers.
5. What should I do if I notice a lump or changes in my breast between screenings?
Answer: If you notice a lump, changes in breast size or shape, skin changes (such as dimpling or puckering), nipple discharge (other than breast milk), or any other unusual symptoms or concerns in your breasts between screenings, it’s essential to contact your healthcare provider promptly. These changes may require further evaluation, which could include additional imaging tests or a clinical breast examination to determine the cause and appropriate course of action. Early detection and timely evaluation of breast changes are crucial for effective breast cancer management.
