COPD
Blanket Health We Have Your Medical Needs Covered!
- Home
- COPD
Understanding COPD: Causes, Symptoms, Diagnosis, and Management
Chronic Obstructive Pulmonary Disease, or COPD, is a progressive respiratory condition that affects millions of people worldwide. It encompasses a group of lung diseases, primarily chronic bronchitis and emphysema, which lead to breathing difficulties and reduced lung function over time. COPD is a significant global health concern, and understanding its causes, symptoms, diagnosis, and management is essential for both patients and healthcare professionals. In this comprehensive article, we will delve into the various aspects of COPD to provide a better understanding of this debilitating condition.
I. Causes and Risk Factors
COPD develops gradually, and its primary causes are long-term exposure to irritants that damage the lungs. The most common risk factors and causes of COPD include:
1. Smoking: Cigarette smoking is the leading cause of COPD. It is responsible for approximately 85-90% of all COPD cases. The harmful chemicals in tobacco smoke irritate and inflame the airways, leading to lung damage over time.
2. Environmental Exposures: Prolonged exposure to indoor air pollutants, such as secondhand smoke, indoor cooking fumes, and workplace dust or chemicals, can contribute to the development of COPD. Occupational hazards like asbestos and coal dust also pose a risk.
3. Genetic Factors: In rare cases, a genetic condition known as alpha-1 antitrypsin deficiency can lead to COPD. This genetic deficiency affects the body’s ability to protect the lungs from damage.
II. Symptoms of COPD

COPD is characterized by a range of symptoms that tend to worsen as the disease progresses. Common symptoms include:
1. Shortness of Breath: One of the earliest and most noticeable signs of COPD is shortness of breath, especially during physical activity. Over time, even simple tasks like climbing stairs or walking short distances can become challenging.
2. Chronic Cough: Many individuals with COPD develop a persistent cough, often accompanied by mucus production. This cough may be worse in the morning.
3. Excess Mucus: COPD can lead to an increase in mucus production in the airways, which can contribute to coughing and difficulty breathing.
4. Wheezing: Wheezing, a high-pitched whistling sound when breathing, is another common symptom of COPD. It occurs as a result of narrowed airways.
5. Chest Tightness: People with COPD often describe a feeling of tightness or discomfort in the chest, especially during physical exertion.
III. Diagnosis and Staging
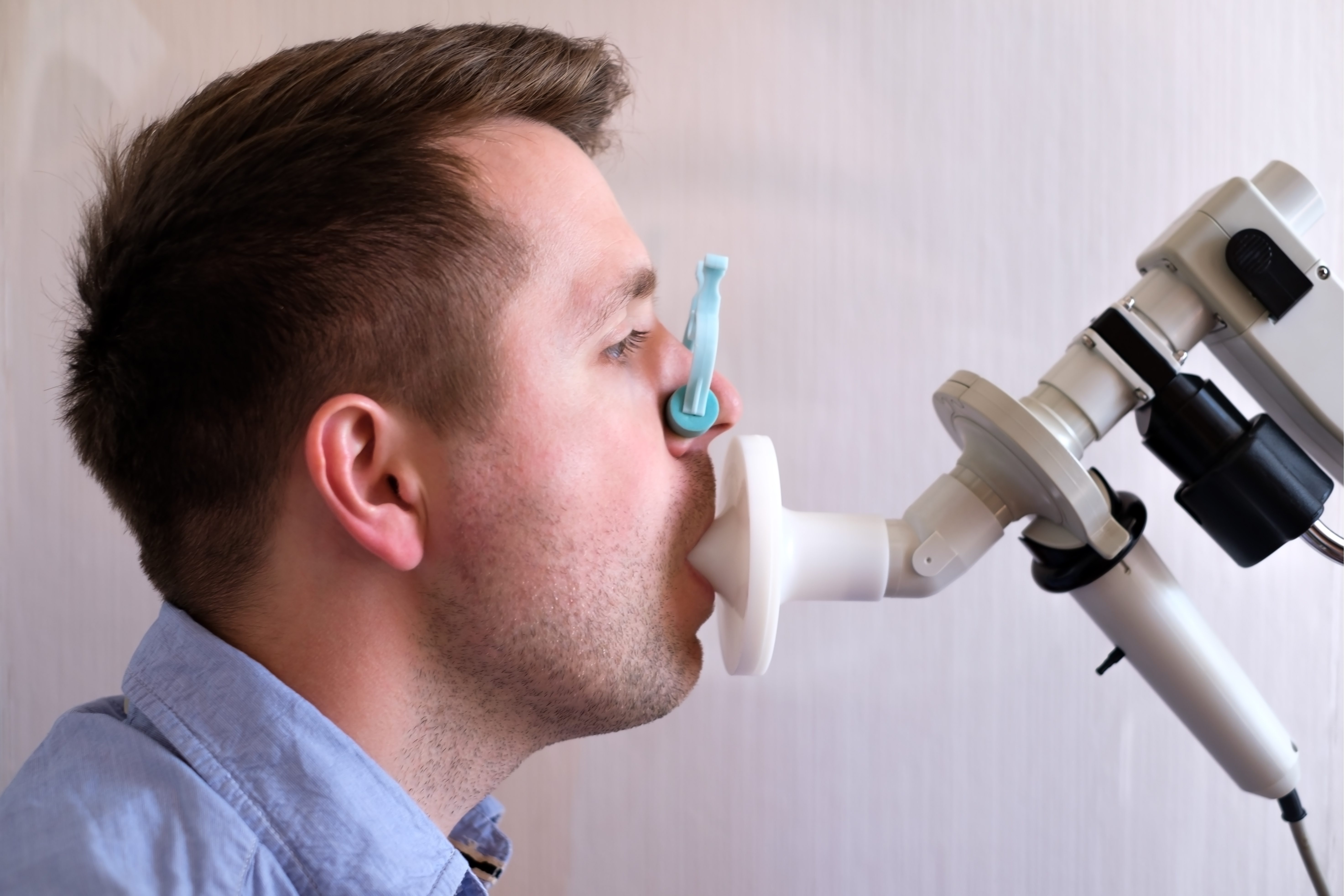
Diagnosing COPD typically involves a combination of medical history, physical examination, and specialized tests. Healthcare providers use spirometry, a lung function test, to measure the amount of air you can exhale and how quickly you can do it. Other tests may include chest X-rays, CT scans, and arterial blood gas analysis.
COPD is typically classified into four stages based on the severity of symptoms and lung function:
1. Stage 1 (Mild): In the initial stage, lung function is still relatively normal, and symptoms may not be very noticeable. Shortness of breath during physical activity is common.
2. Stage 2 (Moderate): As COPD progresses to this stage, lung function begins to decline. Symptoms become more apparent, and daily activities may be affected.
3. Stage 3 (Severe): Severe COPD leads to a substantial decrease in lung function, resulting in more severe symptoms and frequent exacerbations.
4. Stage 4 (Very Severe): At this advanced stage, lung function is significantly impaired, and patients experience severe limitations in daily activities. Respiratory failure is a concern.
IV. Management and Treatment
While there is no cure for COPD, there are various treatment options available to manage symptoms, improve quality of life, and slow disease progression. Treatment plans are tailored to each individual’s specific needs and may include the following components:
1. Lifestyle Modifications: Lifestyle changes are essential for managing COPD. Quitting smoking is the most critical step, as it can slow down the progression of the disease. Avoiding exposure to lung irritants and maintaining a healthy diet and regular exercise routine can also help.
2. Medications: Medications are prescribed to alleviate symptoms and reduce inflammation in the airways. Bronchodilators, which relax the muscles around the airways, and inhaled corticosteroids are commonly used. Some individuals may require oxygen therapy to maintain adequate oxygen levels in the blood.
3. Pulmonary Rehabilitation: Pulmonary rehabilitation programs offer a structured approach to exercise, education, and emotional support for individuals with COPD. These programs can help improve physical fitness and provide strategies for managing symptoms.
4. Vaccinations: Getting vaccinated against influenza and pneumonia is crucial for people with COPD, as they are at higher risk for respiratory infections that can exacerbate their condition.
5. Surgical Interventions: In severe cases of COPD, surgical options such as lung volume reduction surgery or lung transplantation may be considered. These procedures are typically reserved for those who do not respond well to other treatments.
V. Coping with COPD

Living with COPD can be challenging, but it’s important to remember that with proper management and lifestyle adjustments, individuals can lead fulfilling lives. Here are some coping strategies for those with COPD:
1. Education: Educate yourself about COPD and its management. Understanding your condition can empower you to take control of your health.
2. Support: Seek support from healthcare professionals, support groups, or counselors. Sharing experiences and learning from others can be invaluable.
3. Medication Adherence: Take your prescribed medications as directed by your healthcare provider to manage symptoms and prevent exacerbations.
4. Lifestyle Changes: Embrace a healthy lifestyle, including regular exercise, a balanced diet, and stress management techniques.
5. Communication: Keep open lines of communication with your healthcare team. Report any changes in symptoms promptly and follow up on recommended treatments and appointments.
COPD is a chronic lung condition that requires ongoing management, but it should not define the entirety of an individual’s life. With early diagnosis, proper treatment, and lifestyle adjustments, people with COPD can enjoy an improved quality of life and continue to engage in activities they love. It is essential to prioritize lung health, seek support, and follow a comprehensive care plan to manage COPD effectively and enhance overall well-being. By understanding COPD and taking proactive steps, individuals can take control of their health and look forward to a fulfilling future.
Recognizing COPD Symptoms and When To Ask For Help
Recognizing the symptoms of Chronic Obstructive Pulmonary Disease (COPD) is crucial for early diagnosis and effective management of this chronic lung condition. COPD is a progressive disease that primarily includes two main conditions: chronic bronchitis and emphysema. While symptoms can vary from person to person, they typically share common characteristics that become more pronounced as the disease progresses. One of the hallmark symptoms of COPD is shortness of breath, which often begins subtly, particularly during physical exertion. This shortness of breath can initially be dismissed as a result of aging or being out of shape. However, if you find yourself becoming increasingly breathless during activities that previously posed no problem, it could be an early sign of COPD.
Chronic cough is another prevalent symptom of COPD. Individuals with COPD often develop a persistent cough that can be particularly bothersome in the mornings. This cough is usually productive, meaning it produces mucus or phlegm. Over time, the cough may become more frequent and interfere with daily life. Wheezing, characterized by a high-pitched whistling sound when breathing, is another common symptom of COPD. It occurs as a result of narrowed airways, which makes it difficult for air to flow freely. Wheezing can be especially noticeable during physical activity or when exhaling. Chest tightness is also a symptom frequently reported by individuals with COPD. It is described as a sensation of pressure or discomfort in the chest, often associated with shortness of breath. This tightness can vary in intensity and may worsen during periods of exacerbation.

While these symptoms are indicative of COPD, they can overlap with other respiratory conditions, making diagnosis challenging without proper evaluation. Therefore, if you experience any of these symptoms, especially if they persist or worsen over time, it is essential to seek medical help promptly. Knowing when to ask for help is a critical aspect of managing COPD effectively. If you are at risk due to factors such as smoking history, exposure to lung irritants, or a family history of lung disease, it becomes even more important to be vigilant about symptoms. Additionally, if you are already diagnosed with COPD, monitoring for any changes in symptoms is crucial.
Seek medical attention if you notice an escalation in the frequency or severity of your symptoms, as this could indicate a COPD exacerbation. During exacerbations, symptoms such as increased coughing, more significant mucus production, worsening shortness of breath, or chest pain may occur. Exacerbations can be serious and require immediate medical intervention to prevent further lung damage. Another crucial point to consider is the impact of COPD symptoms on your daily life. If you find that your symptoms are limiting your ability to perform routine activities, it’s time to consult a healthcare professional. Whether it’s affecting your ability to exercise, work, or engage in social activities, these limitations should not be dismissed as a natural consequence of aging or lifestyle.
In summary, recognizing the symptoms of COPD and knowing when to ask for help are essential steps in managing this chronic lung condition. Shortness of breath, chronic cough, wheezing, and chest tightness are common indicators of COPD, but they can often be mistaken for other issues. Therefore, it’s crucial to seek medical evaluation if you experience these symptoms, especially if they persist, worsen, or significantly impact your daily life. Early diagnosis and proper management can help improve your quality of life and slow the progression of COPD.
Living with COPD
Living with COPD (Chronic Obstructive Pulmonary Disease) requires making certain lifestyle adjustments to manage symptoms and improve overall well-being. While there are activities that individuals with COPD should avoid to minimize respiratory distress and exacerbations, there are also activities that can be beneficial in aiding their condition.
Activities to Avoid:
Smoking: The most critical action for individuals with COPD is to quit smoking if they are smokers. Smoking is the leading cause of COPD and exacerbates symptoms. Avoiding exposure to secondhand smoke is equally important.
Excessive Physical Exertion: Strenuous physical activities that lead to breathlessness should be avoided. Overexertion can strain the already compromised lungs and lead to exacerbations. It’s essential to engage in moderate, well-paced activities and incorporate rest breaks.
Polluted Air and Allergens: Individuals with COPD should avoid areas with poor air quality, pollution, or allergens that can trigger respiratory symptoms. This includes staying away from heavy traffic, smoke-filled environments, and places with high pollen levels.
Extreme Temperatures: Extreme cold or hot weather can be challenging for individuals with COPD, as temperature extremes can worsen symptoms. It’s advisable to stay indoors during extreme weather conditions or use appropriate protective clothing.
Sick Contacts: COPD patients should avoid close contact with individuals who have respiratory infections, including the common cold and flu. Infections can exacerbate COPD symptoms and lead to hospitalization.
Activities to Aid COPD:
Pulmonary Rehabilitation: Participating in a pulmonary rehabilitation program can be immensely helpful for individuals with COPD. These programs offer structured exercise, education, and emotional support, all aimed at improving lung function and overall well-being.
Breathing Exercises: Practicing breathing exercises, such as pursed-lip breathing and diaphragmatic breathing, can help improve lung function and reduce shortness of breath. These exercises can be learned through pulmonary rehabilitation or with the guidance of a respiratory therapist.
Regular Exercise: Engaging in regular, low-impact exercise is beneficial for COPD patients. Activities like walking, swimming, and cycling can help improve cardiovascular fitness and muscle strength, making breathing easier.
Maintaining a Healthy Diet: Eating a balanced diet rich in fruits, vegetables, lean proteins, and whole grains provides essential nutrients and can help maintain a healthy weight. Being overweight can strain the respiratory system.
Medication Adherence: Following prescribed medication regimens is crucial for managing COPD. Bronchodilators and anti-inflammatory medications can help alleviate symptoms and reduce the frequency of exacerbations.
Vaccinations: Receiving recommended vaccinations, including the flu vaccine and pneumonia vaccine, is essential for preventing respiratory infections that can exacerbate COPD symptoms.
Adequate Hydration: Staying well-hydrated helps maintain mucus thinness in the airways, making it easier to clear mucus and reduce coughing.
Monitoring Symptoms: Keeping track of symptoms and noting any changes is essential. This allows for early intervention in case of exacerbations or worsening symptoms.
Support Groups: Joining COPD support groups or online communities can provide emotional support, practical advice, and a sense of belonging, which can be invaluable for managing the emotional aspects of living with COPD.
Consulting Healthcare Professionals: Regular check-ups with healthcare providers, including primary care physicians and pulmonologists, are essential. They can monitor the progression of COPD, adjust treatment plans, and provide guidance on managing symptoms.
In summary, individuals with COPD should avoid activities that can worsen symptoms or expose them to respiratory irritants. At the same time, they should actively engage in activities that promote lung health, such as pulmonary rehabilitation, breathing exercises, and a healthy lifestyle. With proper management and lifestyle adjustments, COPD patients can lead fulfilling lives and maintain their well-being. Always consult with healthcare professionals for personalized advice on managing COPD.
COPD FAQ
1. What is COPD, and what causes it?
Answer: COPD stands for Chronic Obstructive Pulmonary Disease. It is a progressive lung disease characterized by chronic bronchitis and emphysema, which cause airflow obstruction and breathing difficulties. The primary cause of COPD is long-term exposure to lung irritants, with cigarette smoke being the leading risk factor. Other factors include exposure to environmental pollutants, workplace dust and chemicals, and genetic factors such as alpha-1 antitrypsin deficiency.
2. What are the common symptoms of COPD?
Answer: The common symptoms of COPD include:
- Shortness of breath, especially during physical activity.
- Chronic cough, often with mucus production.
- Wheezing (a high-pitched whistling sound during breathing).
- Chest tightness or discomfort.
- Frequent respiratory infections.
- Fatigue.
- Unintended weight loss.
3. Can COPD be cured?
Answer: No, COPD is a chronic, progressive condition, and there is no cure. However, with proper management and lifestyle changes, individuals with COPD can control symptoms, slow the progression of the disease, and improve their quality of life. Treatment typically includes medications, pulmonary rehabilitation, and lifestyle modifications such as smoking cessation.
4. How is COPD diagnosed?
Answer: COPD is diagnosed through a combination of medical history, physical examination, lung function tests, and imaging studies. Spirometry, a lung function test, is a key diagnostic tool. It measures how much air you can exhale and how quickly you can do it. Other tests, such as chest X-rays and CT scans, may be used to assess lung damage and rule out other conditions.
5. What is the best way to manage COPD?
Answer: The management of COPD involves several key strategies:
- Quitting smoking is the most critical step for smokers.
- Medications, such as bronchodilators and inhaled corticosteroids, can help alleviate symptoms and reduce inflammation.
- Pulmonary rehabilitation programs offer exercise, education, and support to improve physical fitness.
- Lifestyle modifications, including a healthy diet, regular exercise, and avoiding lung irritants, are essential.
- Vaccinations, like the flu and pneumonia vaccines, can prevent respiratory infections.
- Regular follow-up with healthcare providers is crucial for monitoring and adjusting treatment plans.
Remember that COPD management should be personalized, and individuals should work closely with their healthcare team to develop a plan that suits their specific needs and stage of the disease.
