Diabetes Mellitus Type 1 & 2
Blanket Health We Have Your Medical Needs Covered!
- Home
- Diabetes Mellitus Type 1 & 2
Understanding Diabetes Mellitus: Types 1 and 2
Diabetes mellitus, commonly referred to as diabetes, is a chronic medical condition that affects millions of people worldwide. It is characterized by elevated blood sugar levels, which can lead to a range of health complications. Diabetes exists in several forms, but the two most prevalent types are Type 1 and Type 2 diabetes. In this comprehensive article, we will delve into the differences, causes, symptoms, management, and prevention strategies for these two types of diabetes.
I. Diabetes Mellitus: An Overview
Diabetes mellitus is a metabolic disorder that occurs when the body’s ability to regulate blood sugar (glucose) levels is impaired. Glucose is a crucial source of energy for cells, and its absorption and utilization depend on the hormone insulin, produced by the pancreas. When the body fails to produce sufficient insulin or effectively utilize it, blood sugar levels rise, leading to diabetes.
II. Type 1 Diabetes
A. Causes and Mechanism
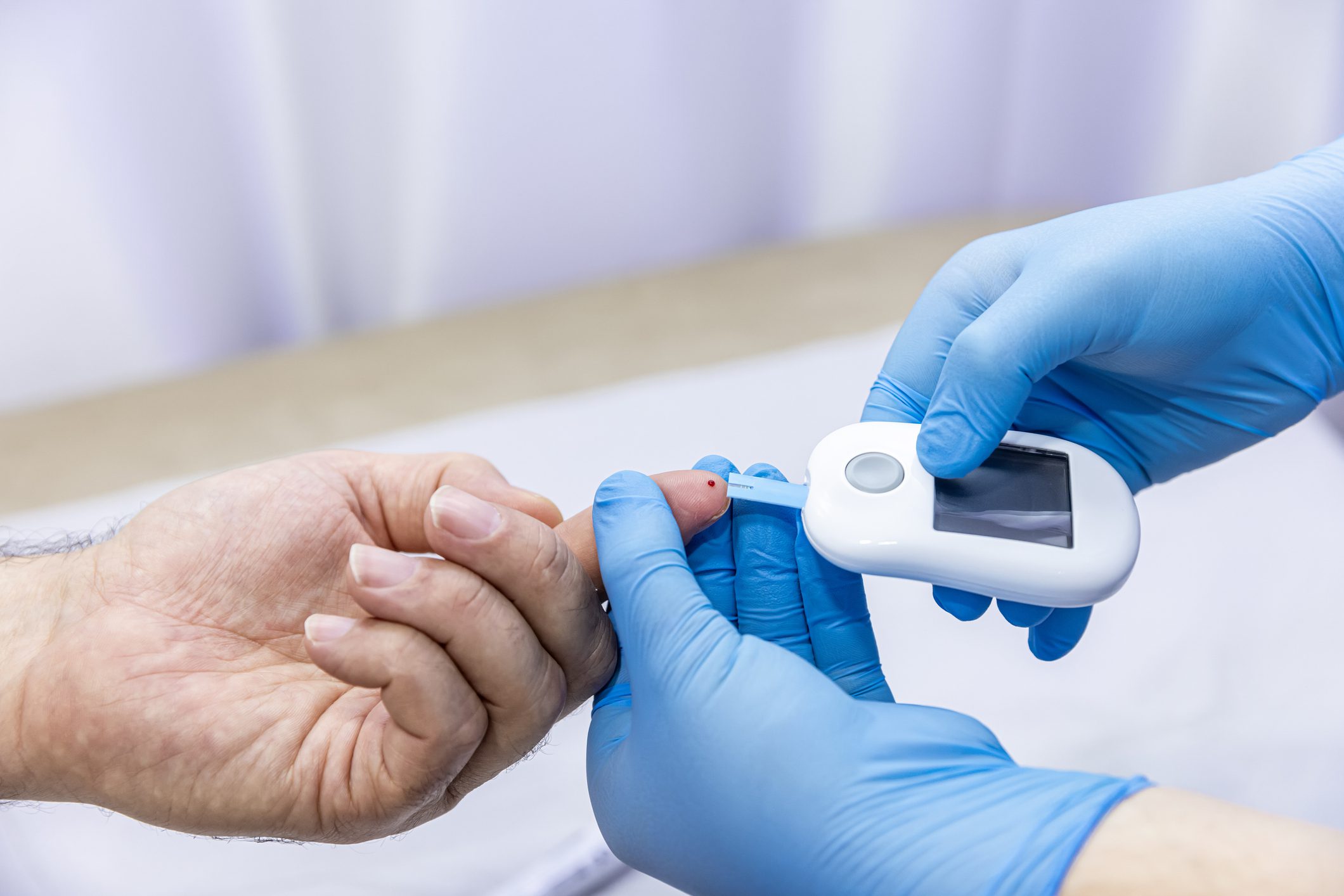
Type 1 diabetes, often referred to as juvenile-onset diabetes or insulin-dependent diabetes, typically develops early in life, although it can occur at any age. This form of diabetes is an autoimmune condition in which the immune system mistakenly attacks and destroys insulin-producing beta cells in the pancreas. As a result, the body cannot produce insulin.
B. Symptoms
Symptoms of Type 1 diabetes may appear suddenly and include:
- Excessive thirst and hunger
- Frequent urination
- Unexplained weight loss
- Fatigue
- Blurred vision
- Increased susceptibility to infections
- Irritability
C. Treatment and Management
Management of Type 1 diabetes requires daily insulin therapy, usually administered through injections or an insulin pump. The goal is to regulate blood sugar levels and mimic the body’s natural insulin production. Regular blood sugar monitoring is essential to adjust insulin doses and maintain target levels. A balanced diet, regular physical activity, and close medical supervision are also crucial aspects of Type 1 diabetes management.
III. Type 2 Diabetes
A. Causes and Mechanism
Type 2 diabetes, often called adult-onset diabetes, is the most common form of diabetes, typically developing later in life, although it is increasingly being diagnosed in younger individuals. In Type 2 diabetes, the body still produces insulin, but the cells become resistant to its effects, causing blood sugar levels to rise.
Several factors contribute to Type 2 diabetes, including genetics, obesity, sedentary lifestyle, poor diet, and age. Obesity, in particular, is a significant risk factor, as excess body fat, especially around the abdomen, can lead to insulin resistance.
B. Symptoms
Symptoms of Type 2 diabetes may develop gradually and include:
- Increased thirst and hunger
- Frequent urination
- Fatigue
- Blurred vision
- Slow-healing wounds and infections
- Tingling or numbness in extremities
- Recurrent skin infections
C. Treatment and Management
The management of Type 2 diabetes primarily focuses on lifestyle modifications and, in some cases, oral medications or insulin therapy. Lifestyle changes include adopting a healthy diet, engaging in regular physical activity, losing excess weight, and managing stress. Medications may be prescribed to improve insulin sensitivity or stimulate insulin production. Regular blood sugar monitoring and routine medical check-ups are essential to monitor progress and adjust treatment plans accordingly.
IV. Key Differences Between Type 1 and Type 2 Diabetes
- Causes: Type 1 diabetes is an autoimmune disorder resulting from the destruction of insulin-producing beta cells, whereas Type 2 diabetes is primarily influenced by genetic factors, obesity, and insulin resistance.
- Age of Onset: Type 1 diabetes typically begins in childhood or adolescence, whereas Type 2 diabetes often develops in adulthood, though it is becoming more common in younger individuals due to rising obesity rates.
- Insulin Dependency: Individuals with Type 1 diabetes require lifelong insulin therapy from the time of diagnosis. In Type 2 diabetes, some individuals may manage their condition with lifestyle changes and oral medications, while others may eventually require insulin.
- Symptoms: Symptoms of Type 1 diabetes often appear suddenly and include extreme thirst, frequent urination, and weight loss. Type 2 diabetes symptoms tend to develop gradually and may include fatigue, blurred vision, and slow wound healing.
- Prevention: Type 1 diabetes cannot be prevented, as it is an autoimmune condition. However, Type 2 diabetes can often be prevented or delayed through lifestyle modifications, including weight management, healthy eating, and regular physical activity.
V. Prevention and Risk Reduction
 Preventing Type 1 diabetes is not currently possible, as it is believed to result from genetic and environmental factors beyond our control. However, for Type 2 diabetes, prevention and risk reduction are achievable through the following strategies:
Preventing Type 1 diabetes is not currently possible, as it is believed to result from genetic and environmental factors beyond our control. However, for Type 2 diabetes, prevention and risk reduction are achievable through the following strategies:
- Maintain a Healthy Weight: Achieving and maintaining a healthy weight can significantly reduce the risk of Type 2 diabetes. Losing excess weight, especially around the abdomen, improves insulin sensitivity.
- Adopt a Balanced Diet: Emphasize a diet rich in whole grains, fruits, vegetables, lean proteins, and healthy fats. Minimize the consumption of sugary, processed foods and sugary beverages.
- Regular Physical Activity: Engage in regular physical activity, such as brisk walking, swimming, or cycling, for at least 150 minutes per week. Exercise helps control blood sugar levels and improves insulin sensitivity.
- Limit Alcohol Consumption: If you choose to drink alcohol, do so in moderation. Excessive alcohol consumption can contribute to insulin resistance.
- Don’t Smoke: Smoking is associated with an increased risk of Type 2 diabetes. Quitting smoking can improve overall health and reduce diabetes risk.
- Regular Check-Ups: Periodic medical check-ups can help monitor blood sugar levels and identify any potential issues early. If you have risk factors for Type 2 diabetes, discuss preventive measures with your healthcare provider.
Diabetes mellitus, encompassing Type 1 and Type 2 diabetes, is a complex chronic condition that affects millions of individuals worldwide. While Type 1 diabetes is an autoimmune disorder requiring lifelong insulin therapy, Type 2 diabetes is closely linked to lifestyle factors and often manageable through lifestyle modifications and, in some cases, medication. Both forms of diabetes benefit from early detection and appropriate management to prevent complications and promote overall well-being. Understanding the differences between these two types and adopting preventive measures can help reduce the risk of developing Type 2 diabetes and improve the quality of life for those affected by either form of the condition.
Recognizing The Symptoms of Diabetes Mellitus
Recognizing the symptoms of diabetes mellitus is crucial for early diagnosis and effective management of this chronic condition. Diabetes mellitus encompasses two primary types: Type 1 and Type 2. Both types share some common symptoms, while others may vary. Here’s a detailed guide on how to recognize the symptoms of diabetes mellitus:
Common Symptoms of Diabetes Mellitus (Type 1 and Type 2):
Frequent Urination (Polyuria): One of the hallmark symptoms of diabetes is excessive urination. High blood sugar levels cause the kidneys to work overtime to filter and remove excess glucose from the bloodstream, leading to increased urine production. Individuals with diabetes may find themselves visiting the bathroom more frequently, including waking up during the night to urinate.
Excessive Thirst (Polydipsia): The increased urination associated with diabetes can lead to dehydration, triggering intense thirst. People with diabetes often find themselves drinking more fluids than usual in an attempt to quench their thirst.
Increased Hunger (Polyphagia): Despite eating regularly, individuals with diabetes may experience persistent hunger. This occurs because the body’s cells are not effectively using glucose for energy, leading to a sense of hunger.
Unexplained Weight Loss: Diabetes can lead to unintended weight loss, particularly in Type 1 diabetes. As the body lacks the ability to use glucose for energy, it starts breaking down fat and muscle tissues. This leads to weight loss even when calorie intake is normal or increased.
Fatigue: Persistent fatigue and low energy levels are common symptoms of diabetes. Glucose is the body’s primary energy source, and when it cannot enter cells efficiently due to insulin resistance or lack of insulin, it results in feelings of tiredness and weakness.
Symptoms More Common in Type 1 Diabetes:
 Sudden Onset: Type 1 diabetes often develops rapidly, with symptoms appearing abruptly. This can include a sudden increase in thirst, urination, and hunger, as well as significant weight loss over a short period.
Sudden Onset: Type 1 diabetes often develops rapidly, with symptoms appearing abruptly. This can include a sudden increase in thirst, urination, and hunger, as well as significant weight loss over a short period.
Ketosis: In Type 1 diabetes, the body may enter a state called ketosis, where it breaks down fat for energy. This can lead to the production of ketones, which can cause fruity-smelling breath, nausea, and even diabetic ketoacidosis (DKA) if left untreated. DKA is a severe and potentially life-threatening condition that requires immediate medical attention.
Symptoms More Common in Type 2 Diabetes:
Gradual Onset: Type 2 diabetes tends to develop more gradually, with symptoms appearing slowly over time. Many people with Type 2 diabetes may not even notice symptoms for years.
Blurred Vision: High blood sugar levels can affect the lenses in the eyes, leading to blurry or distorted vision. This symptom is more common in Type 2 diabetes and often improves with blood sugar control.
Frequent Infections and Slow Healing: People with Type 2 diabetes may experience frequent infections, such as urinary tract or skin infections, and slower wound healing. Elevated blood sugar levels can weaken the immune system and impair the body’s ability to fight infections.
Tingling or Numbness: Nerve damage (neuropathy) is a common complication of Type 2 diabetes. It can lead to tingling or numbness in the extremities, particularly the hands and feet.
Itching and Skin Changes: Diabetes can cause skin issues like dryness, itching, and dark patches on the skin, especially in skin folds and around the neck.
Recognizing these symptoms is essential, as untreated diabetes can lead to severe complications such as cardiovascular disease, kidney damage, nerve damage, and vision problems. If you or someone you know is experiencing these symptoms, it’s crucial to seek medical attention promptly. Early diagnosis and proper management can help individuals with diabetes live healthy and fulfilling lives while reducing the risk of complications.
Diabetes Mellitus Types 1 & 2 FAQ
1. What is the difference between Type 1 and Type 2 diabetes?
Answer: Type 1 diabetes is an autoimmune condition where the immune system attacks and destroys insulin-producing beta cells in the pancreas. This results in a lack of insulin production. Type 2 diabetes, on the other hand, typically develops later in life and involves insulin resistance, where the body’s cells do not respond effectively to insulin, and eventually, the pancreas may not produce enough insulin.
2. Can diabetes be prevented?
Answer: Type 1 diabetes cannot currently be prevented, as it is believed to result from genetic and environmental factors beyond our control. However, Type 2 diabetes is often preventable or manageable through lifestyle modifications such as maintaining a healthy weight, eating a balanced diet, engaging in regular physical activity, and managing stress.
3. How is diabetes diagnosed?
Answer: Diabetes is diagnosed through blood tests that measure fasting blood sugar levels and/or hemoglobin A1c levels, which provide an average of blood sugar levels over several months. A diagnosis is typically made if fasting blood sugar levels are consistently above 126 mg/dL (milligrams per deciliter) or hemoglobin A1c levels are 6.5% or higher.
4. What are the treatment options for diabetes?
Answer: Treatment for diabetes varies depending on the type and severity. For Type 1 diabetes, treatment involves lifelong insulin therapy, often administered through injections or an insulin pump. Type 2 diabetes management typically starts with lifestyle modifications, including a healthy diet, regular exercise, and weight management. In some cases, oral medications or insulin therapy may also be prescribed.
5. What are the potential complications of diabetes?
Answer: Diabetes, if poorly managed, can lead to various complications, including cardiovascular disease, kidney damage (nephropathy), nerve damage (neuropathy), vision problems (retinopathy), foot problems, and skin conditions. It can also increase the risk of infections and slow wound healing. However, with proper management and blood sugar control, the risk of complications can be significantly reduced.
It’s important to note that diabetes is a complex condition, and individuals should consult with healthcare professionals for personalized guidance and treatment plans based on their specific circumstances.
